What type of insulin goes into an insulin pump?
Table of contents
Do you have diabetes and are curious about insulin pumps? Are you struggling with daily injections? You can’t get your blood sugar levels to the correct level? Insulin pumps can offer lifestyle freedom and flexibility, so it’s no surprise you want to know more. There are many types of insulin pump brands on the market that can cause confusion. Read on to find out about the different types of insulin pumps available and the pros and cons of using pumps. You can use this information to talk with your healthcare provider, or your Diabetes Care and Education Specialist to work out which option is right for you.
Why are insulin pumps used?
You can think of an insulin pump as a human pancreas supplying your body with doses of insulin. When you have type 1 diabetes the only choice of medication is insulin. If you have type 2 diabetes you may use insulin injections if diet and tablets are not working for you.
For some people and you may be one of them, an insulin pump could be just what you need to get your blood sugar levels to target and reduce episodes of hypoglycemia. These devices are as close as you can currently get to the gradual administration of rapid-acting insulin that is normally taking place in the body. Insulin pump therapy may be the answer for patients who can not achieve good blood glucose levels with syringes, insulin pens, or insulin jet injectors.
How does an insulin pump work?
All pumps look like a small device about the size of a mobile phone and run off batteries with an inbuilt alarm to warn you if the battery is running low. There are many insulin pump brands on the market. The one you choose will depend on various factors. Speak with your healthcare provider to figure out which option is right for you.
When you use an insulin pump to treat your diabetes two different types of insulin dosages are used:
Basal
The rate at which insulin slowly enters your body is called the basal rate. Basal insulin is given to you continuously throughout the day and night. Your basal insulin is usually a small amount and can vary depending on your needs e.g. if you are exercising. You determine your individual basal rates by measuring your blood sugar levels with a blood glucose meter. Most people check blood sugar at least four times a day, or you may use a continuous glucose monitor (CGM). Many insurance companies require you to take readings four times a day as a policy.
Bolus
At mealtimes, you can push a button to deliver extra insulin called a bolus dose. You determine this amount by carbohydrate counting. Bolus insulin is a rapid-acting insulin. Your Diabetes Care and Education Specialist will help you with calculating insulin doses and the amounts of boluses based on your carbohydrate intake, and how to set the pump. Most pumps also have a bolus calculator function to help you.
What types of insulin pumps are there?
The best type of insulin pump depends on your lifestyle. The two main options available are a traditional pump or a tubeless pump (patch pump). Both types of pumps are attached to your body by a tiny tube called a cannula. Your cannula needs to be changed every 2-3 days regardless of which type of pump you use. Additionally, it is very important you move your cannula to a different part of your body each time you use it, to prevent injection bruises and bumps.
Traditional Insulin pumps
The parts that make up a traditional insulin pump
- Insulin reservoir (or container) with a pumping mechanism
- Tubing to attach to the body
- Infusion set
The pump body contains buttons that allow you to program various bits of information e.g. amount of insulin for meals, specific types of basal rates, or stop the insulin infusion. The pump itself can be carried on your belt or pocket. If you want to hide it you can wear it under your clothes.
Insulin patch pumps
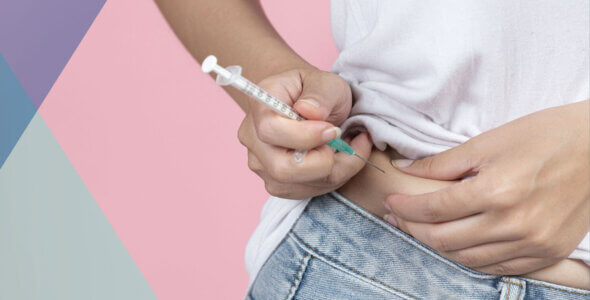
These are worn directly on the body and attached with an adhesive patch. Inside is a small case that contains a reservoir pumping mechanism, and an infusion set that is attached to a site on the body e.g. abdominal, leg, or arm. Patch pumps have no extra tubing which means the pump sits directly on your skin. It is controlled wirelessly by a separate device that allows the programming of insulin delivery.
Here are some examples of commonly used FDA approved insulin pumps:
- Medtronic: Medtronic offers the Minimed 770G system (approved for type 1 diabetes for ages 2 and older) and the Minimed 630G system (approved for both type 1 and type 2 diabetes for ages 14 and older)
- Omnipod: The Omnipod DASH system can be used by children and adults for both type 1 and type 2 diabetes
- Tandem: Tandem makes the t:slim X2 insulin pump. This pump is intended for people with type 1 diabetes who are ages 6 and older
The pros and cons of insulin pumps
Pros
- It often smoothes out the swings of glucose during the day because the insulin is administered slowly and in small doses
- It is flexible because you can take the bolus dose just before a meal
- You do not need to take daily injections
- You can rapidly disconnect and reconnect the pump to take a shower or swim but it can take a little getting used to when worn to bed
- It’s safe from overdosage because it has built-in proactive devices to prevent this from happening
Cons
- Infections of the skin are possible because the infusion set is left in place for several days
- Frequent testing of blood glucose is essential, at least four times a day (unless your pump has an inbuilt system for testing)
- Only short-acting insulin is used in the pump so if insulin stops you may enter ketoacidosis rapidly
- You may be allergic to the tape that holds the infusion set onto the skin
- Commitment, time, and training is needed to use your pump correctly
Diabetes technology is a great way forward in diabetes management but requires a lot of time and effort, to begin with, and using a pump is definitely not a treatment to do on your own at the beginning. The American Diabetes Association state the one requirement for using a pump is that you and your caregivers are ready and willing to do what it takes to use the pump safely. You will need hands-on training from your diabetes care team. You will be taught how to fill a pump reservoir, prime tubing, select an infusion site, change an infusion set, disconnect the device, calculate and program insulin doses, fix potential problems, create backup plans in case of pump failure, and prevent diabetic ketoacidosis.
Medically reviewed
A medical professional has reviewed this article.


Jamie Winn, PharmD
Jamie Winn, PharmD
Dr. Jamie Winn received his Doctor of Pharmacy in 2002 from the University of South Carolina College of Pharmacy, Columbia, SC. Jamie is a medical reviewer for NiceRx.