Best type of insulin pumps
Table of contents
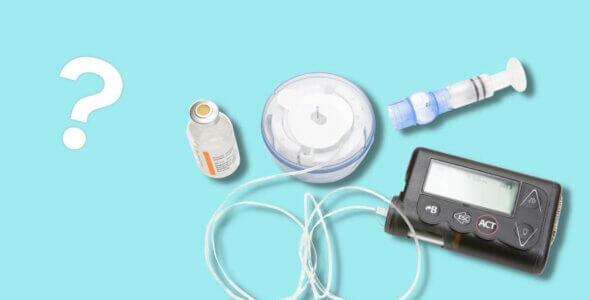
Insulin pumps are part of the rapid progression in diabetes management. In 2019 a review found over 350,000 people in the United States were using insulin pump therapy (also known as continuous subcutaneous insulin infusion (CSII) to control their diabetes. New technology to manage your diabetes can be overwhelming! Maybe you’ve just started using your insulin pump and you’re still getting to grips with your equipment and have some unanswered questions. Maybe you are in the early stages of considering an insulin pump. One area of confusion is what type of insulin is used in which pump.
How does insulin work?
The most important hormone to understand in diabetes is insulin. It is made in your pancreas which is located just behind your stomach.
Without getting too medical let’s look at how insulin works. Insulin travels in your blood through your body. It opens up cells in your body so that glucose can enter them. After glucose enters cells, the cells immediately use it for energy in the form of glycogen or convert it to fat for use later. When glucose leaves your blood and enters cells, your blood glucose level falls. Your pancreas detects your glucose falling and turns off the release of insulin. This stops your blood sugar from going too low and causing hypoglycemia. At the same time, your liver begins to make more glucose in your blood.
This whole system keeps your glucose levels correct. Insulin is the only means that the body has of lowering blood glucose levels. When this system fails diabetes occurs. Each type of diabetes involves the pancreas not functioning properly.
When you have type 1 diabetes the only choice of medication is insulin. If you have type 2 diabetes you may use insulin injections if diet and tablets are not working for you. Insulin pumps are an option for both types of diabetes.
How does insulin for pumps work?
The job of an insulin pump is to provide continuous delivery of insulin all day long. An insulin pump can replace your daily injections or long-acting insulin injections. This is because an insulin pump releases insulin when the body needs it, it works like a human pancreas. The settings on a pump allow the doses of insulin to be adjusted therefore you can tailor your insulin delivery.
A rapid-acting insulin is used in insulin pumps, occasionally Regular insulin. Rapid-acting insulin types are aspart (NovoLog), lispro (Humalog), and glulisine (Apidra). The reason for using short-acting insulin is that the pump can deliver a steady amount of insulin called basal insulin all day long. In addition at mealtimes, a bolus amount of insulin can be easily delivered with just a push of a button.
Let us look at the terms basal insulin and bolus insulin in more depth to understand how the insulin pump works to treat your diabetes.
Basal
The rate at which insulin slowly enters your body is called the basal rate. Basal insulin is given to you continuously throughout the day and night. Your basal insulin is usually a small amount and can vary depending on your needs e.g. physical activity. You determine your individual basal rates by measuring your blood sugar levels with a blood glucose meter. Most people check their blood sugar at least four times a day or may use a continuous glucose monitor (CGM). Many insurance companies require you to take readings four times a day as a policy.
Bolus
At mealtimes, you can push a button to deliver extra insulin called a bolus dose. You determine this amount by using your blood glucose reading and the amount of carbohydrate you plan on eating. Your Diabetes Care and Education Specialist will help you with calculating insulin doses and the amounts of boluses based on your carbohydrate intake, and how to set the pump. Sounds like too many calculations? Most pumps also have a bolus calculator function to help you.
Final word
We hope this blog has provided you with an answer to what type of insulin goes into an insulin pump and helps clear up any confusion. Remember your healthcare team is there to help and guide you with your insulin pump. You will need hands-on training from your healthcare team to operate your pump. You will be taught how to fill a pump reservoir, prime tubing, select an infusion site, change an infusion set, disconnect the device, calculate and program insulin doses, fix potential problems, create backup plans in case of pump failure, and prevent diabetic ketoacidosis.
Medically reviewed
A medical professional has reviewed this article.


Jamie Winn, PharmD
Jamie Winn, PharmD
Dr. Jamie Winn received his Doctor of Pharmacy in 2002 from the University of South Carolina College of Pharmacy, Columbia, SC. Jamie is a medical reviewer for NiceRx.