What is Insulin Uses, warnings & interactions
Complete a free online enrollment application to find out if you’re eligible to pay only $49 per month for your Insulin medication.
Get started todayInsulin is a hormone that your body makes naturally. It’s produced by beta cells in your pancreas, a small organ found behind your stomach. Your pancreas secretes the insulin it makes into your bloodstream.
What does insulin do?
Insulin has two main functions, both of which help you to maintain a healthy blood sugar level.
When you digest food and drink, a type of sugar called glucose is released into your blood. The glucose is taken around your body in your bloodstream so it can be delivered to the cells that use it for energy. Insulin in your blood helps your cells absorb glucose. Insulin molecules attach to the surface of your cells, triggering them to bring glucose transporting proteins to the surface, which bring glucose into the cell.
If you have more glucose in your blood than your cells need, insulin also signals your liver to absorb and store the excess glucose, so it can be used later when your blood glucose has fallen.
What is diabetes?
Diabetes is a group of diseases that cause you to have too much glucose in your blood for long periods. The two most common forms of diabetes are called type 1 and type 2 diabetes.
Type 1 diabetes, sometimes called insulin-dependent diabetes, is an immune system disorder where your immune system mistakenly attacks healthy tissue in your body. With type 1 diabetes, your immune system targets and destroys the beta cells in your pancreas that make insulin. This means your pancreas doesn’t produce enough insulin, so your blood glucose levels stay higher than is healthy.
With type 2 diabetes, your cells become resistant to insulin, meaning the insulin you produce doesn’t work as well. Your pancreas may also stop producing as much insulin as it should. Both of these cause your cells to absorb less glucose than they should, causing your blood glucose to be too high.
High blood glucose can make you feel hungry, thirsty, and tired, but over time it can cause or contribute to more serious health problems. These can include nerve damage, kidney failure, heart disease, strokes, vision loss, and it can lead to the amputation of parts of your body.
What is insulin resistance?
Insulin resistance is when your muscle, liver, and fat cells stop responding as well to insulin. This means the cells absorb less glucose from your blood in the presence of insulin than they should, causing your blood glucose to be too high. Insulin resistance is a leading cause of type 2 diabetes.
Insulin for the treatment of diabetes
You can take an insulin medication to treat both type 1 and type 2 diabetes. For type 1 diabetes, insulin helps to replace that which is lost when your pancreas doesn’t produce enough. For type 2 diabetes, insulin injections can replace lost insulin and help counter insulin resistance. Insulin is usually used alongside other treatments for type 2 diabetes, like lifestyle changes and sometimes other medication.
How does insulin work?
You take insulin by injecting it under your skin (subcutaneous injection). The injected insulin is then absorbed into your bloodstream and works in the same way as the insulin your pancreas produces. It attaches to the surface of your cells, triggering them to absorb glucose, as well as causing your liver to store excess glucose.
The only important difference between the insulin produced by your pancreas and the insulin you inject is that the injected insulin is sometimes made to be faster acting or longer acting than natural insulin (see Types of Insulin below for more of this).
How effective is insulin for diabetes?
Insulin is a safe and effective treatment for most people with diabetes. If your pancreas isn’t producing enough insulin, or you’ve developed insulin resistance, insulin injections can help your cells absorb more glucose and lower your blood glucose levels. Insulin may be the only medication you need to treat your diabetes, but in some cases, it’s used alongside other treatments, particularly for type 2 diabetes.
Types of insulin
There are many different brands and different types of insulin. They all work in the same way as natural insulin, but they’ve been designed to affect you at different speeds and to last for different lengths of time. Faster acting insulin is usually used after a meal to help absorb the glucose released, whereas longer-acting insulin is used to help lower your blood glucose throughout a whole day.
List of insulin medications
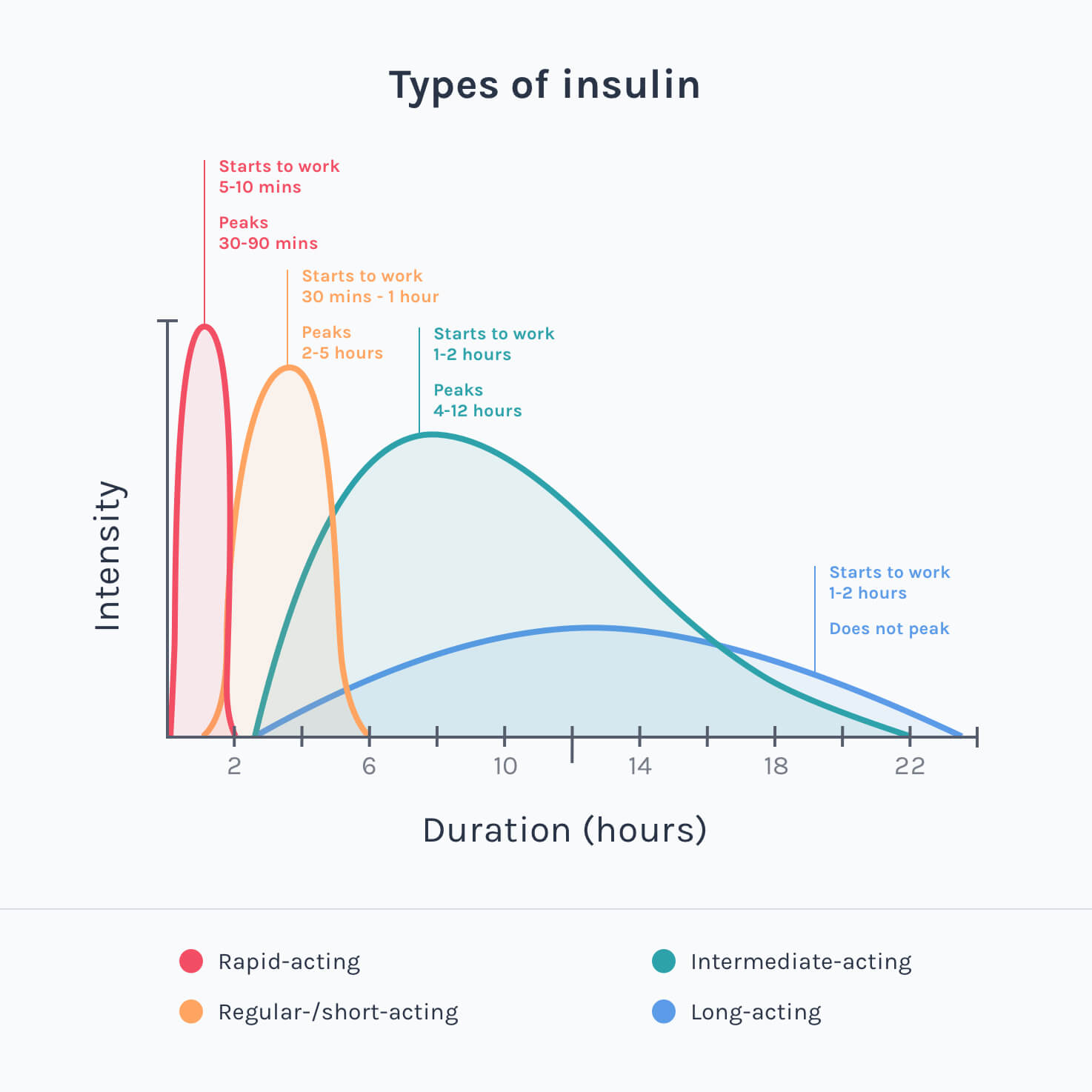
Broadly, you can group insulin brands into five types:
- Rapid-acting insulin starts to work in around five to 30 minutes and lasts for around one to five hours. Examples include:
- Short-acting insulin starts to work in around 30 minutes to one hour and lasts for around two to eight hours. Examples include:
- Intermediate-acting insulin starts to work in around one to two hours and lasts for around 18 to 24 hours. Examples include:
- Long-acting insulin starts to work in around one to three hours and lasts from 20 to 48 hours. Examples include:
- Combination insulin (a blend of insulins, usually a short-acting insulin combined with a longer-acting insulin):
How to take insulin
You take insulin by injecting it under your skin (subcutaneous injection), usually in your stomach, thighs, buttocks, or upper arms. You can do this using either a syringe or a self-injecting pen device, depending on which one you’re more comfortable with. Your doctor or a diabetes educator can show you how to inject insulin or how to use an insulin pen.

You can also take the medication using an insulin pump – a device you wear that has a small tube (cannula) that’s inserted into your skin. The pump can automatically deliver set doses, and some people find it a more convenient alternative to multiple daily injections. Your doctor or a diabetes educator can also demonstrate how an insulin pump works.
Insulin side effects
Just as with any medication, insulin can cause side effects in some people. It is important to note that not everyone will experience side effects. These can also vary by person and by brand of insulin.
However, we can summarize the most common insulin side effects as including the following:
- Reactions at the site of injection (insulin injection side effects), like itching, rashes, skin thickening, or pits forming in your skin (lipodystrophy)
- Allergic reactions that can cause swelling of your face, tongue, or throat
- Swelling of your hands and feet
- Weight gain
Insulin also has the potential to cause more serious side effects. These can include:
- Severe allergic reactions to the medication that can cause anaphylaxis
- Your blood glucose falls too low (hypoglycemia)
- Your blood potassium falling too low (hypokalemia)
- Heart failure – this is more likely if you take insulin alongside another type of medication called TZDs (thiazolidinediones)
This is simply a summary of the side effects that insulin can cause. To find out more, you can read the leaflet that comes with your medication, or you can talk to your doctor.
Is insulin safe for use during pregnancy?
Using insulin during pregnancy is a common concern, but insulin is generally considered the safest diabetes medication you can use when pregnant or when nursing. It doesn’t cross the placenta, so won’t enter your unborn baby’s bloodstream, and it doesn’t pass into your breastmilk. You should talk to your doctor about insulin during pregnancy if you become or want to become pregnant, or if you plan to breastfeed.
How to store insulin?
You can keep the current insulin that you’re using at room temperature to make sure it’s not uncomfortable to inject. Insulin can usually be kept at room temperature for around one month but refer to the patient leaflet that comes with your specific brand of insulin for more details.
You should store any extra insulin in a refrigerator. Make sure you don’t expose any insulin to extremes of hot or cold temperature and keep it out of direct sunlight.
The cost of insulin
Insulin can be a costly monthly expense. The cost of insulin without insurance will vary depending on the brand of insulin you buy and the way it’s administered. Insulin typically comes in pre-filled syringes, in self-injecting pen devices, or in vials to be used in syringes or in an insulin pump. Costs will also vary by retailer.
As a general guide, one self-injecting insulin pen, that can last from around one week to two (depending on the dose you take and the size of the pen) can cost from $80 to $250. The specific price of the prescribed type of insulin with insurance will depend on the terms of your healthcare plan.
If you get your insulin with the help of NiceRx through an insulin patient assistance program, you’ll always pay a flat monthly fee of $49.
Apply online to find out more.
Rationing insulin
The high cost of insulin has led some people with diabetes to ration their insulin – to use less than they should, so it lasts longer.
This is a dangerous and even deadly habit, as it can make the insulin you take to become less effective than is required. Your doctor has prescribed a dose of insulin that they feel is most suitable for you, and you should always take it as they’ve directed.
Alternative (non-insulin) medications for diabetes
Insulin is one medication that can be used to treat diabetes, but there are others. Some of these are used instead of insulin, others can be used alongside insulin. Non-insulin diabetes medications include:
- SGLT2 inhibitors – these medications encourage your body to excrete more glucose in your urine to lower your glucose levels. Examples include
- DPP-4 inhibitors – these drugs slow how quickly your body breaks down insulin, keeping it working for longer. Examples include:
- Alpha-glucosidase inhibitors – these drugs slow how quickly your body releases glucose when you digest food and drink. Examples include:
- Precose
- Glyset
- Glucagon-like peptides – these encourage your pancreas to make more insulin and reduce how much glucose is released into your blood. Examples include:
- Biguanides/metformin reduces the amount of glucose released into your blood and can keep insulin working for longer. Examples include:
- Meglitinides encourage your pancreas to make more insulin. Examples include:
- Starlix
- Prandin
- Sulfonylureas encourage your pancreas to make more insulin. Examples include:
- DiaBeta
- Glucotrol
- Amaryl
- Glucagon is a medication used to treat very low blood sugar. It is also a hormone naturally found in the body. Examples include:
- Glucagon
- Baqsimi
- Glucagon Emergency Kit
- GlucaGen HypoKit
- Gvoke
You can also make a range of lifestyle changes that can help treat type 2 diabetes. These include:
- Losing excess weight
- Getting regular exercise
- Eating a diabetes-friendly diet that helps you lose excess weight and reduces your blood pressure and blood cholesterol
Insulin FAQs
Is insulin a hormone?
Yes, insulin is a hormone that’s naturally produced by your body. It is made by your pancreas – a small organ behind your stomach. The insulin you take as a diabetes medication is also a hormone and works in the same way as the insulin your pancreas produces.
Is metformin insulin?
No, although metformin is used to treat diabetes, it’s not a type of insulin. Metformin is a medication you take to stop your liver from releasing glucose – it helps your cells to absorb glucose more effectively in the presence of insulin.
Does insulin cause weight gain?
Weight gain is a common side effect of insulin. Not everyone will experience this side effect, but some people will. Talk to your doctor if you’re concerned about insulin and weight gain.
Can you get off insulin once you start?
If you have type 1 diabetes, your pancreas produces less insulin, and you may need to take insulin for life. If you have type 2 diabetes, your condition can be reversed if you use diabetes medications, like insulin, and make changes to your lifestyle, like losing excess weight, eating a diabetes-friendly diet, and exercising more. Once your blood sugar is under control, you may be able to reduce your insulin use or stop using it altogether.
What is the safest insulin?
Insulin is the safest diabetes medication for most people with the condition, with all types of insulin considered to be safe. The brand and type of insulin you’re prescribed will usually depend on your insulin requirements, whether you need faster-acting or longer-acting insulin, or a combination of the two.
What are the side effects of insulin?
Insulin can cause side effects, although not everyone will experience them. People will also experience them differently. The more regular insulin side effects include itching and rashes at the site of injection, allergic reactions, and weight gain. Insulin can also cause a range of other side effects – and in rare cases, these can be serious. Talk to your doctor to find out more about insulin side effects.



